Current Employment Status:
Hired Full Time on Feb 13, 2024
Queeny
Medical Biller|Data Entry|Revenue Cycle Management
Profile Description
I am Detail-oriented Medical Billing Specialist with 4 years of experience handling billing and clerical tasks to ensure accurate and timely patient billing. I have excellent knowledge in managing patient accounts and can provide support to clients related to billing with accuracy and confidentiality . During my tenure, I have delivered exceptional results and high-quality service and operational excellence to improve productivity and quality. I can assist your organization in optimizing its revenue cycle by ensuring proper billing and adherence to industry regulations.
SOFT SKILL:
1. Time Management
2.Positive Attitude
3.Negotiation
4.Decision Making
5.Leadership
HARD SKILL:
1. Charge Entry
2. Claims Submission
3. Claims Denials and Rejections
4. A/R Follow ups
5. Familiarity with EMR and EHRs ( eCW, Athena, Kareo/Tebra and Elation)
6. Knowledge of HMOs and Medicaid
• Critical Thinking and Coordination• Able to multi-task to meet timelines on deliverables• Ability to prioritize and meet timelines on deliverables deadlines• Excellent customer service and• Strong attention to detail• Self-starter and can work well interpersonal skills under pressure• Knowledgeable in several different CRMs
I can help you with the following:
*Medical Billing Services
1. Entering patient information, patient financials, type of treatment, CDT/CPT codes, and insurance information into billing software
2. Verifying insurance information via insurance website
3. Submitting claims to Medicaid, Medicare, and other third-party Payers.
4. Following up on unpaid and outstanding balances.
5. Researching and resolving denials and aging reports.
• Perform posting charges
• Ensure patient's medical information is accurate and up-to-date
• Assist in patient's inquiries with benefits, payments, and eligibility
• Perform completion of claims to payers
• Conduct duties in a professional and timely fashion
• Submit billing data to appropriate insurance providers
• Process claims and resolve denials to ensure maximum reimbursement
• Follow up unpaid claims to appropriate parties/ payers
• Do medicare and medi-cal reviews
• Review remits and payer correspondence and escalate any identified issues to
appropriate areas for review and response to expedite claim resolution
• Insurance verification, authorization and appeals
• Analyze EOBs and remits
Let's discuss how I can assist you and your practice!
Top Skills
Customer Support » Insurance » Medical Insurance
Experience: 2 - 5 years
Office and Administration » Data Entry
Experience: 2 - 5 years
Other Skills
Accounting » Accounts Receivable
Experience: Less than 6 months
Customer Support » Insurance
Experience: 2 - 5 years
Office and Administration » Microsoft Excel
Experience: Less than 6 months
Office and Administration » Microsoft Excel
Experience: Less than 6 months
Basic Information
- Age
- 28
- Gender
- Female
- Website
- Sign Up with Pro Account to View
- Address
- Lapu-Lapu, Cebu
- Tests Taken
- IQ
- Score: 132
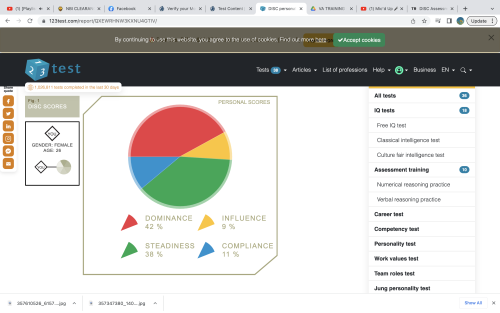
- DISC
- Dominance: 42
- Influence: 9
- Steadiness: 38
- Compliance: 11
- English
- C2(Advanced/Mastery)
- Uploaded ID
- Sign Up with Pro Account to View
“My Filipino specialist who is absolutely amazing..go get your OFS today!”
Eden Einav
SEE MORE REAL RESULTS“The more I stepped away from it, the more successful our Chanel became!”
- Jim Orr
Onlinejobs.ph "ID Proof" indicates if "they are who they say they are".
It DOES NOT indicate skill level.
ID Proof scores are 0 - 99 with 99 being the best. It is calculated based on dozens of data points.
It's intended to help employers know who they're talking to is real, and not a fake identity.


 You have successfully pinned this profile! You can manage pinned profiles in your Employer dashboard.
You have successfully pinned this profile! You can manage pinned profiles in your Employer dashboard.
